National Reality: Hospitals Are Operating at the Edge
According to Becker’s Hospital Review, which referenced Kaufman Hall’s National Hospital Flash Report, hospitals ended 2025 with an adjusted operating margin of only 1.3%.
This number is well below the usual 3 to 4% margin hospitals need to:
- Maintain infrastructure and physical plants.
- Service debt obligations
- Fund baseline technology investments
With a 1.3% margin, hospitals lack financial stability that could lead to a reduction in services or closure.
Kaufman Hall characterizes the financial challenges facing hospitals in 2026 as a “new normal” defined by:
- Rising labor and supply costs
- Increasing bad debt associated with increasing uninsured and underinsured rates
- A deteriorating payer mix with increased payer friction
- A more complex and acute inpatient population
- Persistent margin compression
The Structural Deficit: Service Lines That Lose Money
The American Hospital Association’s (AHA) data show a deeper problem: core hospital services are losing money, regardless of payer.
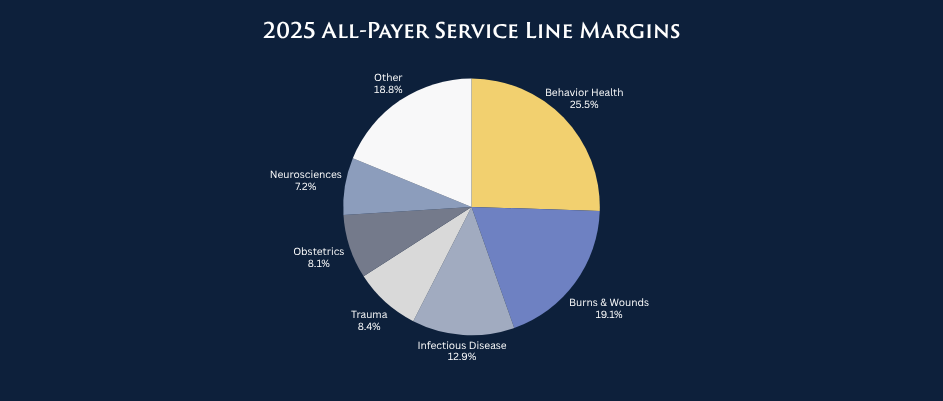
These aren’t optional services. They are essential for community care. Hospitals can no longer offset these shortfalls with profits from other areas.
The Only Remaining Lever: Revenue Cycle Integrity
When core services lose money, and the payer mix worsens, hospitals have only one thing they can control.
Collect their earned revenue and fight hard to keep it. This shifts the revenue cycle from an administrative task viewed as a cost center to a margin-protection strategy. Payer friction is driving up the cost of healthcare. The AHA estimates that revenue cycle function account for as much as 40% of hospital costs. If current trends continue, the cost of collecting earned revenue could exceed the cost of delivering patient care.
Why Physician Advisors Are Now Mission-Critical
Hospitals are trying a variety of strategies, with the most common being the implementation of technology. However, the complexity of the inpatient revenue cycle is proving beyond the capabilities of many of these tools. Human intervention is still required. The bottom line is that hospitals need to expect more from their revenue cycle departments. In this environment, defensibility of clinical decision-making becomes the core asset.
Physician Advisors play a central role by:
- Educating admitting physicians about how to document to support medical necessity and accurate billing.
- Supporting status determinations (inpatient vs. observation) with clinical judgment.
- Conducting peer-to-peer reviews with payer medical directors to overturn adverse determinations.
- Leading appeals that convert denials into revenue recovery.
Successful status upgrades or appeals can yield thousands per case—critical when margins are 1.3%. This is a tangible, immediate benefit that accumulates over time.
Revenue Cycle as a Clinical Strategy
Hospitals that succeed in this environment share a common approach.
They treat the revenue cycle as:
- A clinical function, not purely administrative
- Real-time discipline and accountability, not retrospective cleanup
- A strategic capability, not a cost center
This includes:
- Embedding Physician Advisors into utilization management workflows
- Aligning utilization review, CDI, coding, and clinical documentation practices by breaking down silos
- Using data to identify denial patterns and problematic payer behaviors
The Bottom Line
The convergence of:
- Structurally negative service line margins
- Sub-2% operating performance
- Increasingly aggressive payer tactics
…creates a healthcare environment where: Revenue cycle performance is the margin.
Hospitals are fighting for financial stability, not just small improvements.
Hospitals that invest in physician advisors will protect their revenue. Those that don’t will see their margins shrink even faster.
Final Thought
The future of hospitals depends on decisive action. As financial pressures grow and essential service lines lose money, investing in efficient and effective physician-led revenue cycle strategies is not optional; it is vital. Hospitals that make revenue cycle integrity a top clinical and strategic priority will define the next era of healthcare. Defending every earned dollar is the difference between stability and decline. Organizations that act with urgency will lead; those that hesitate will fall behind, risking their mission and their communities. Now is the moment to lead. Protect your hospital’s future by investing in revenue cycle excellence.
Hospitals cannot afford to leave reimbursement to chance
Connect with Brundage Group to strengthen medical necessity defensibility, reduce denials, and protect every earned dollar.





